Clinical Services
Vasectomy

Clinical Services: Vasectomy
PDF versions available: Clinical Services: Vasectomy (ENG, PDF)
Ref code: 1615-MSIAU-230814
This page contains information about your vasectomy. Read this information carefully and keep it to look at later on. Ask us if you have any questions after reading it.
Things to know
Consent
- It is important that you understand the process, any risks, and that you are sure about your choice.
- Risks of vasectomy are described in the medical risks section.
- We will ask you to give your written consent to the procedure.
- It is important that you understand our fees and charges so you can give informed financial consent.
If you do not understand anything in this document, if you have any questions, or if you feel that you’re being pressured or coerced, please let us know.
Interpreter services
Please let us know if you need a telephone interpreter to help you understand any of this information. If you need one at any time before or after your procedure, you can call: TIS National on 131 450 and ask to be connected to us on 1300 003 707.
Make a complaint or provide feedback
If you would like to provide any feedback, you can:
- talk to any staff member at the clinic
- write directly to the clinic
- call our National Contact Centre on 1300 003 707
- use our feedback form on the homepage of our website.
If we don’t satisfy your concerns, you may also escalate your complaint to the independent body in your State.
What is a vasectomy?
Vasectomy is the common name for male sterilisation—a permanent method of contraception.
A vasectomy involves cutting and separating the ends of the tubes (vas deferens) that move sperm from the testicles to the penis. After the procedure, (once you have the all-clear after approximately 3 months) ejaculated semen will contain no sperm.
Sperm is the part of semen that leads to pregnancy, and after a vasectomy it will be broken down in your body instead of making its way into your semen.
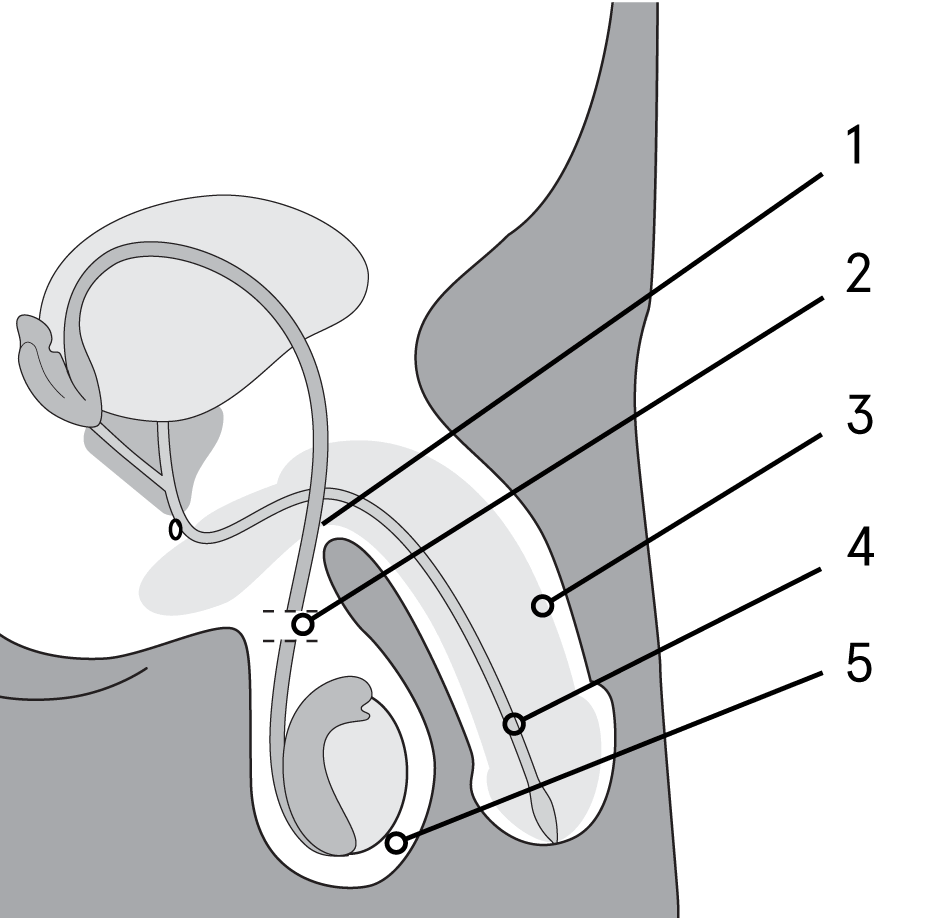
Illustration key:
- Vas deferens
- Vasectomy
- Penis
- Urethra
- Testes
Before your vasectomy
Preparing for your vasectomy
Pre-admission phone call
Before your appointment, you will have a consultation on the phone with a nurse to discuss your medical history and how to prepare you for your procedure.
Sedation
If you’re having IV sedation, please read the sedation information booklet to make sure you follow the fasting rules correctly before your procedure.
Stopping some medications
- Stop taking any form of aspirin, fish oil and non-steroidal anti-inflammatory drugs (nsaids) including ibuprofen (nurofen) for 7 days before and 7 days after your procedure.
- If you are taking anticoagulant (blood thinning) medication, we strongly recommend stopping this for up to 7 days before your procedure and for 7 days after your procedure, but you must talk to your GP or specialist about how to do this.
- You can use this page as a reference when discussing this with them.
Do not stop taking anticoagulant (blood thinning) medication without talking to your doctor, as this may put your health at risk.
Hair removal
You will need to shave or have someone else help you shave the following areas no more than 24 hours before your procedure. Try and shave on the morning of your procedure.
- Do not shave more than 24 hours before your procedure as it may increase the risk of infection.
- Shave the entire scrotum as well as 1-2cm up the shaft and the sides of the penis from the scrotum.
- Include any long hairs that can reach to the front of the scrotum.
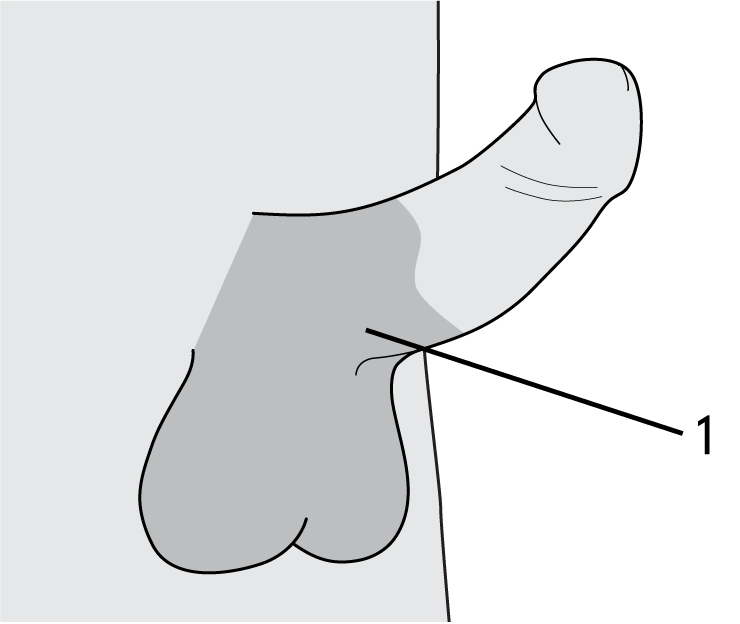
Illustration key:
- Area to be shaved
While you are at the clinic
Expect to spend 2–4 hours at our clinic, depending on the type of anaesthetic you have chosen.
You will have a consultation with your doctor before the procedure. Your partner or support person is welcome to be with you during the consultation.
- We will ask you about your decision to have a vasectomy.
- We will ask about your medical history, especially any past surgeries on your testicles or hernia repair.
- We will explain the procedure, as well as the risks.
- You’re welcome to ask any questions you might have.
We will provide you with aftercare instructions, a pathology form and a specimen jar for your sperm count test. The doctor will examine you to make sure that both your vas deferens can be felt.
What happens during my procedure?
- You will change into a gown before entering the procedure room.
- Your support person will not be able to be stay with you during the procedure.
- They may prefer to leave the clinic and return later.
- We will give you your chosen anaesthetic before the procedure starts.
- If you are having IV sedation, it’s important to read the information in the sedation information booklet.
- Once the doctor has given you a local anaesthetic to numb the area, the doctor will make a small opening in the skin of your scrotum to access your vas deferens and close the upper end.
- In most cases, no scalpel is used and there are no external stitches needed.
- A small dressing is put on at the end of the procedure.
- The procedure usually takes no more than 15 minutes.
After you leave the clinic
Your recovery is important
If your work involves a lot of sitting, you can go back to work 1-2 days after your vasectomy. Please see the ‘return to activity’ section at the bottom of this page for more information.

Up to 2-3 days after vasectomy
You should rest as much as possible for the first day or so. Do not stand and walk much.
- You should wear tighter fitting briefs, as they are more supportive than boxers.
- Use cold therapy regularly to reduce swelling and help with healing.
See cold therapy in the pain management section at the bottom of this page.

Up to 1 week after vasectomy
No swimming or baths for the first week after your operation. Keep the wound as dry as possible.
Have quick showers (in and out) and keep the dressing in place for the full week, if possible.
- Only replace with a new dressing if it is lifting off.
- No heavy or physical activities.
- No sex or ejaculation.
- You may have 1-2 alcoholic drinks per day, but do not drink more than this.
After your procedure
Below are some things you may feel after your procedure. If you’re worried about anything, please call our free aftercare line on 1300 888 022.

Pain
The anaesthetic will wear off a few hours after the procedure. You may feel some pain or aching for 1-3 days. See the pain management section for tips on how to relieve pain.
Call us on 1300 888 022 if you have strong pain, or you are concerned about the pain.

Swelling and bruising
Most people will have some bruising and swelling around the testicles. If your swelling continues, you can use cold therapy to treat it.
- A small pea-sized lump called a granuloma may develop on the cut end of the vas deferens internally.
- It generally shrinks after 6-12 months.
- Do not squeeze these lumps. If you do squeeze them, they may become more painful or swollen.
See cold therapy in the simple guidelines section at the bottom of this page. Call us on 1300 888 022 if the wound has not healed after 2 weeks.

Wound site
If your wound opens to a diamond shaped opening do not be concerned, it will still heal but will now take 2 weeks to close. Keep it as dry as possible during this time.
Call us on 1300 888 022 if the wound has not healed after 2 weeks.

Bleeding
You may have a small amount of bleeding from the vasectomy wound. To stop the blood flow:
- wash your hands
- pinch the skin edges of the wound together very firmly with your finger and thumb
- hold it very tightly for 5 minutes.
You may get a few drops of blood in your ejaculate during the first 1-2 months after your vasectomy. This is normal. Do not be concerned if this happens.
Call us on 1300 888 022 if the bleeding does not stop, or if blood in ejaculate continues more than 2 months after your vasectomy or is very heavy (ejaculate becomes red).
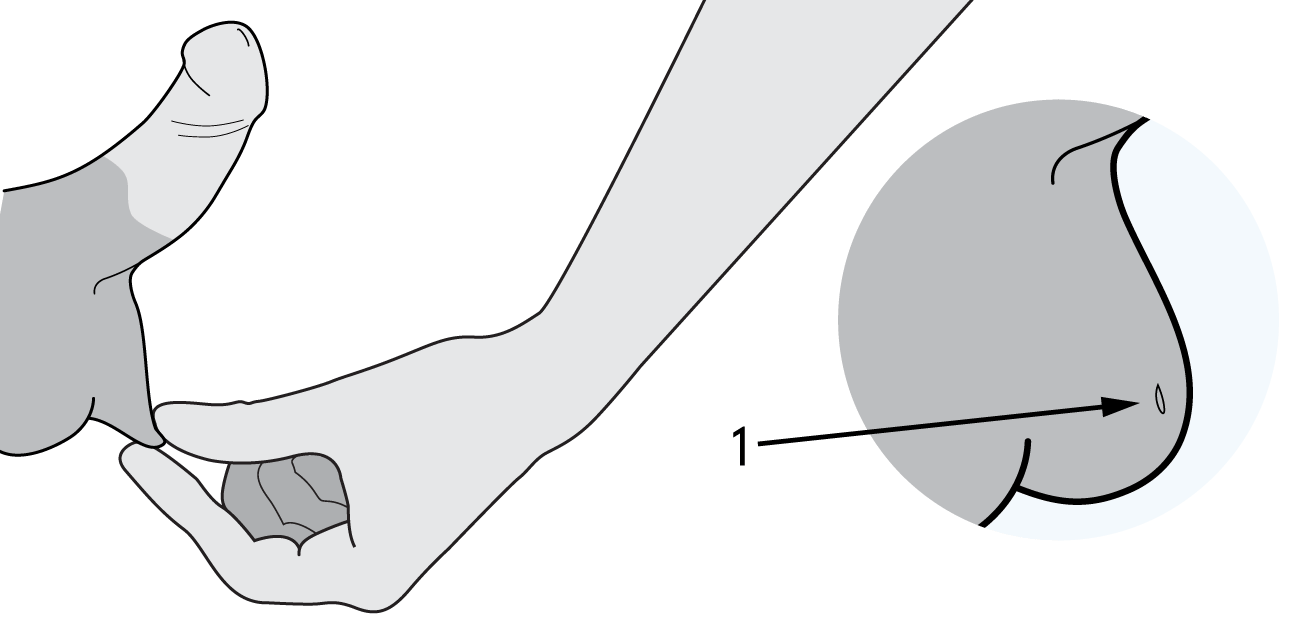
Illustration key:
- Wound site
Pain management
If you have pain when you get home, you can use these pain management techniques.

Medication
You can take pain relief, such as paracetamol (e.g. Panadol). Follow the directions on the packaging and do not take more than instructed. Avoid ibuprofen or aspirin for the first 7 days as these can increase bleeding and bruising.

Cold therapy
You should use cold therapy regularly for the first 3 days while you are awake. If you have swelling after this time, you can keep using cold therapy to help treat it.
- Place a cold pack, cold compress or frozen peas wrapped in a cloth on top or under the scrotum, leaving your underpants and/or your pants on.
- Do not apply cold pack directly to your skin, as this can damage your skin and cause more pain.
- Try to keep it on for as long as possible. If it becomes uncomfortable it is too cold.
- You don’t need to freeze the area, just keep it cooler.

Supportive clothing
Close fitting briefs or trunks may help reduce discomfort and swelling during the first 3 days after your vasectomy.
Surgical risks
Like all surgical procedures, a vasectomy does have some risks.
The risks below do not include all possible complications but are the more common or important complications.
Infection
Risk: less than 1 in 100 procedures.
What is it: when bacteria enters the body and causes disease. Infections involving the skin of the scrotum are not common. Deeper infections may occur around the site of the vasectomy operation internally and may produce a painful, large lump.
Action/treatment: if you develop, redness and/or heat in the scrotum and/or fever, this requires urgent medical assessment. Infection is treated with antibiotics.
Failure
Risk: our technique that we use has an early failure rate of less than 1 in 1000.
What is it: the ends of the vas deferens may grow back together, making you fertile again. This usually occurs in the first 1 to 2 months (early failure) and should show up in your sperm count. In rare cases the vas deferens may re-join after a clear sperm count (late failure).
Action/treatment: we can repeat the vasectomy at no cost to you. Continue using contraception until your vasectomy is successful.
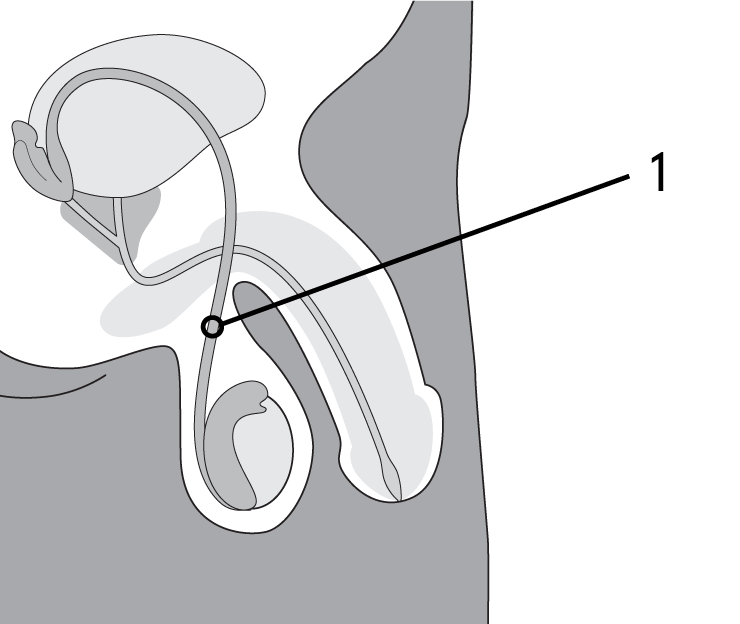
Illustration key:
- Vas deferens have grown back again
Haematoma
Risk: less than 1 in 100 procedures.
What is it: when blood collects deep inside the scrotum, causing swelling and pain. This is most likely during the first 1-2 weeks after your vasectomy. The chances may be higher with physical activity or direct injury.
Action/treatment: it usually settles by itself with rest and support. If it is large, the haematoma may need to be surgically drained. If the haematoma has become solid, it cannot be drained and can take 2-3 months to breakdown and reabsorb.
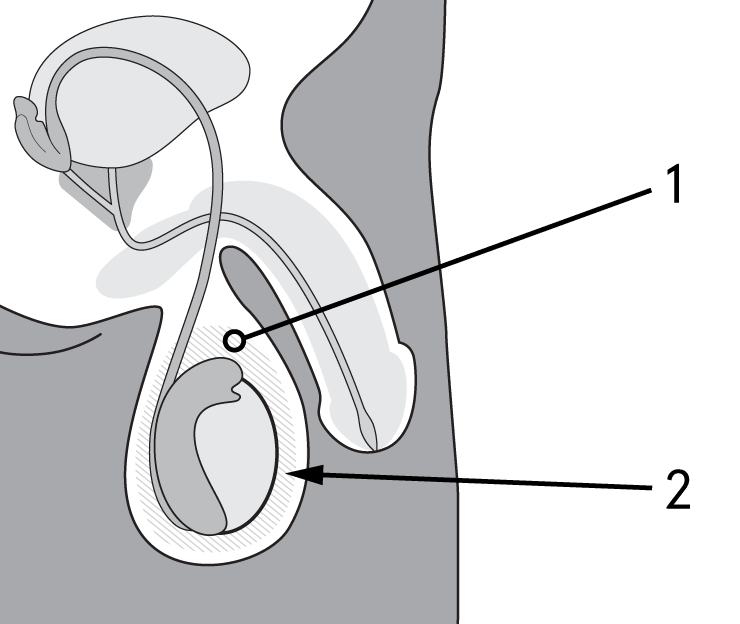
Illustration key:
- Haematoma
- Swollen testes
Granuloma
Risk: less than 1 in 100 procedures.
What is it: a hard, sometimes painful, lump about the size of a pea, sometimes caused by sperm leaking from the cut vas deferens. The lump is not serious and usually shrinks over 6-12 months.
Action/treatment: do not squeeze the lump as you can make it worse. Take simple painkillers when you need them. If it doesn’t get better over time the granuloma can be surgically removed.

Post vasectomy pain syndrome
Risk: around 1 in 300 procedures.
What is it: chronic pain in the scrotum, groin and/or lower abdomen following vasectomy that lasts longer than 3 months. The exact cause is unknown, but it may be related to nerve sensitivity and/or sperm granulomas and/or chronic congestive epididymitis.
Action/treatment: usually responds to pain relief medication and settles by itself. Very occasionally additional surgery is required.

Congestion
Risk: Up to 14 in 100. The open-ended vasectomy technique which we use reduces the risk.
What is it: a sense of pressure caused by sperm build up in the testes and epididymis. It can cause some discomfort for up to 3 months or longer after your vasectomy.
Action/treatment: It should get better with time and painkillers.
Semen analysis and aftercare
Your vasectomy will not be effective straight away.
It is very important that you use another method of contraception during sex until your semen is free of sperm.
Remember, condoms are the only method of contraception that protect against sexually transmitted infections.
Semen analysis
3 months after your vasectomy, you will need to do a semen test. You cannot do it earlier. Your sample is checked under a microscope to see if there are any sperm left.
To help make sure sperm are cleared out before your test, we recommend at least 25 ejaculations before providing a sample.
Click here for a guide to Post Vasectomy Semen Analysis Requirements.
- ACT & NSW: Laverty Pathology
- QLD & Northern NSW: QML Pathology
- SA: Abbott Pathology
- VIC: Dorevitch Pathology
- WA: Western Diagnostics Pathology
Collecting your semen sample
Do not ejaculate for 3 to 4 days before collecting the sample. Collect the entire sample by ejaculating directly into the container provided. Label the container ‘post-vasectomy,’ with your full name, date of birth and time of collection.
Do not:
- use lubricants
- pull out during sex
- collect from a condom
- refrigerate your sample
Your results
Once we have received and reviewed your results, we will contact you to let you know whether your semen is free of sperm. This will usually happen 14-18 days after submitting your sample.
Until we confirm your semen is free of sperm, you need to keep using contraception to prevent pregnancy.
If you have questions about your results, please call our National Contact Centre on 1300 003 707. Please do not call the clinic directly, they will not be able to access your results.
Return to activity
If your work involves any kind of lifting, reaching or other physical exertion you will need to follow these guidelines. If this is not possible, you will need to take the week off work. Remember to ask for a medical certificate during your consultation, if required.
Day 1
- do not lift anything over 3kg
- walk and stand for 5 minutes at a time only
- take 10 to 15-minute rest breaks
Days 2-7
- you can increase walking and standing by 30 minutes each day until day 7
- take 10 to 15-minute rest breaks
Days 7-13
- you can walk and stand all day
- lift 10-15kgs carefully
- no sport yet
Days 14-20
- you can play sports like running, swimming, cycling on a stationary bike (in a gym)
- lift 20-30kgs carefully
Days 21-27
- You can cycle on the road
Day 28
- you can play contact sports like football
- lift and press heavy weights over 30kgs
- do heavy leg press, squats, power lifting
- do martial arts
- do mountain biking
Care and support before, during and after your procedure
Call us on 1300 003 707 for any questions about your appointment.
For medical concerns call our aftercare line 1300 888 022.
If you need a telephone interpreter to help, you can call TIS National on 131 450 and ask to be connected to the service you need.
Your Healthcare Rights
MSI Australia adopts the Australian Charter of Healthcare Rights. The Charter provides a framework of client rights which allows clients, families, carers and services providing health care to work together towards a safe and high quality health system, achieving the best possible outcomes.
The Charter is guided by the following principles:
- Access
- Safety
- Respect
- Partnership
- Information
- Privacy
- Give feedback
As a client of MSI Australia, you have a right to:
- be treated in a professional, courteous, and caring manner
- be respected regardless of your gender, age, sexual orientation, disability, religion, and cultural and linguistic diversity
- have your concerns, complaints and suggestions taken seriously.
If we don’t satisfy your concerns, you may also escalate your complaint to the independent body in your State.
For more information about your healthcare rights and the Charter, head to safetyandquality.gov.au.
This page last edited: August 2023
Ref: 1615-MSIAU-230814
